You are here
To Be Old, Frail And Evicted: Patients at Risk
As Nursing Homes Shift Focus To Short-Term Rehab Care, Families Must Look Elsewhere
- This article was cited as a Story of Note in the 2009 book Covering the Health of Local Nursing Homes, by Charles Bell and Bob Rosenblatt and published by Center for Excellence in Health Care Journalism and the Association of Health Care Journalists.
- This article was recognized in 2009 with the Jack Newfield Award for Investigative Reporting, from the Friends and Relatives of the Institutionalized Aged, as noted in a post on AHCJ's Covering Health blog.
Since Jasmine Nguyen collapsed nine years ago, apparently from a seizure, the 32-year-old has lived in a nursing home in Lodi, Calif., dependent on a ventilator to breathe and the facility's staff for her daily needs.
But since early this year, the nursing home has been seeking to evict Ms. Nguyen and a dozen other residents in similar situations, potentially replacing them with shorter-term residents likely to bring more revenue.
Across the country, nursing homes are forcing out frail and ill residents. While federal law permits nursing-home evictions in some circumstances, state officials and patient advocates say facilities often go too far, seeking to evict those who are merely inconvenient or too costly. Residents with dementia or demanding families are among the most vulnerable, particularly if -- like Ms. Nguyen and the other Lodi residents -- they depend on Medicaid to pay their bills, the officials and advocates say.
Those on Medicaid bring facilities as little as half what they can get from residents who pay out of pocket, with private health insurance or through Medicare, the federal-state health program for the elderly.
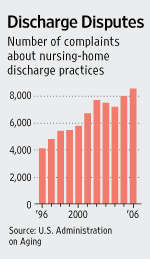
No one counts evictions nationwide. But formal complaints about nursing-home discharge practices have doubled over a decade, to 8,500 nationally in 2006, making it the second-biggest category tracked by the federal Administration on Aging, trailing only complaints about unanswered calls for assistance.
Iowa officials say involuntary discharges have risen even as the number of nursing-home beds has declined. In the District of Columbia, officials contest roughly one in seven evictions as improper, and say still more go unchallenged. Officials in more than a dozen other states echo their stories.
"Across the board, involuntary discharge numbers have risen in recent years," says Louise Ryan, Washington state's long-term-care ombudsman, or official resident advocate. "It's a real problem."
And evictions may be even more widespread, since some eviction attempts are resolved without formal complaints. Residents may not know they can appeal or may be too ill to do so or fear retribution. "It's really hard to know how many folks were simply told, 'We think you need to find another place for your mother,' " says Robyn Grant, long-term-care policy director with United Senior Action of Indiana, an Indianapolis advocacy group.
The nursing-home industry argues that evictions are uncommon, and justified when they occur. Mark Reagan, a California attorney for nursing homes and a state trade association, says most evictions involve dangerous or hard-to-care-for residents that the facilities aren't equipped to handle, or residents who "just don't pay." The American Health Care Association, a national nursing-home trade group, says it isn't aware of broad problems with involuntary discharges, much less ones focusing on Medicaid residents.
Federal law -- enforced by the states -- says residents can be discharged involuntarily for just six reasons: if they are well enough to go home; need care only available elsewhere; endanger the health of others; endanger the safety of others; fail to pay their bills; or if a facility closes its doors. Even so, nursing homes must give residents at least 30 days' notice, explain their appeal rights, and put together a plan to make sure the move doesn't harm them.
'Objectionably Untidy'
But they don't always follow the rules. In a recent review of admission agreements at Missouri nursing homes, nearly one in five granted itself the right to evict residents without cause, the National Senior Citizens Law Center found. Almost half the agreements authorized eviction for residents who become "uncooperative and unmanageable," "unduly noisy," "objectionably untidy" or for other reasons not permitted under federal law.
Nursing homes rarely roll evicted residents out to the curb. Instead, they transfer them to another nursing home or send them to a hospital or psychiatric facility for treatment and observation, and then refuse to take them back, a practice hospital social-workers sometimes call "nursing-home dumps."
"They basically don't want to deal with them," says Cara Pacione, social-work director for 291-bed Mount Sinai Hospital in Chicago, which sees two or three patients sent by nursing homes each month who are refused readmittance.
Even an orderly eviction can carry grave risks for the old and ill. Studies suggest "transfer trauma," or relocation-stress syndrome, can spur depression and weight loss and increase the risk of falls.
"Transfer trauma kills elderly, frail people," says Esther Houser, Oklahoma's long-term-care ombudsman for more than 25 years. After a small nursing home in her state closed suddenly last fall, 10 of the 16 relocated residents were dead by early March, she says. "People get lost, people don't know which side of the bed to get out of, or where the bathroom is."
Louis VanderLinde, a retired college professor in Frankfort, Mich., lived just six weeks after the Maples, a county-owned nursing home there, evicted him.
The facility knew he had Alzheimer's disease when it admitted him three years before, but last summer gave his wife, Nancy, 30 days to find him a new home. When she couldn't find one nearby, the Maples drove him 160 miles to a nursing home in Lincoln, Mich.
He fell within a half-hour, and soon suffered two bouts with pneumonia after inhaling food at meals; he died Oct. 12. "You could see the panicky look in his eyes -- everything was strange," Mrs. VanderLinde says. "It's a terrible thing to live through."
Marsha Latour, chairwoman of the board of the Maples, declined to comment on specifics of the VanderLindes' experience, citing patient confidentiality. She said Mr. VanderLinde's condition had reached a point that, without a dedicated Alzheimer's unit, the Maples was "not able to take care of him." The Maples ultimately released him to another facility that also lacked a dedicated Alzheimer's unit.
Like many of those served with eviction notices, Mr. VanderLinde was on Medicaid. Roughly two-thirds of those who remain in a nursing home 90 days or longer depend on Medicaid, having exhausted their own savings or other benefits. But nursing-homes are increasingly concentrating on patients coming off hospital stays and therefore eligible for Medicare benefits or private insurance, says Michael Wiederhorn, a health-care analyst for Oppenheimer & Co. "That's what they're all doing right now, is building up these recovery-rehab units."
The move makes good financial sense: Sun Healthcare Group Inc., a publicly traded chain with more than 200 long-term care facilities in 25 states, says it averages $411 a day from Medicare patients -- but just $166 from those on Medicaid. A recent industry estimate says Medicaid's rates, established separately by each state, fell $4.4 billion short of what it cost nursing homes to care for residents on the program's rolls last year alone.
Often, nursing homes cite one of the federally permitted reasons to evict residents, but advocates for the elderly say it can be a stretch.
Closed -- For Renovations
For example, the nursing home hoping to evict Jasmine Nguyen, Lodi Memorial Hospital, told her and a dozen others in February that they would have to move by June 30 because the nonprofit organization was closing the facility -- for renovations.
All 13 residents were "sub-acute" patients, most of them dependent on ventilators or feeding tubes, or with other conditions requiring significant extra care.
Lodi Memorial told the state it planned to replace them with patients recently discharged from its hospital -- who typically require shorter-term care covered at a higher daily rate by private insurance or by Medicare. (Medicare pays for up to 100 days in a nursing home following a hospital stay of at least three days.)
"They're not closing the facility," says Patricia McGinnis, executive director of California Advocates for Nursing Home Reform.
In April, after Lodi Memorial sought state approval, administrators were told that they knew when admitting the sub-acute residents that they would need extensive care, probably for many years, and it couldn't simply stop. Moreover, the state said in a letter, "your facility is not ceasing to operate as you are not surrendering your license."
Lodi Memorial has asked the state to reconsider. Spokeswoman Carol Farron says the facility described its plans as "ceasing to operate" because none of the options under federal rules quite fit, so "we had to pick the one that best met the circumstances." The move is unrelated to reimbursement, she adds. She says the hospital is now considering using the space for inpatient hospital beds, if the sub-acute residents can be moved.
The nearest nursing home certified to care for patients like Ms. Nguyen is about two hours away with traffic, says Jasmine's 23-year-old sister, Mary. Their mother, Kim Nguyen, who runs the family nail salon in nearby Stockton, visits Jasmine twice a day.
"I think it would kill her if she couldn't see my sister," Mary Nguyen says.
When residents fight an eviction, they often win, according to lawyers for both nursing homes and residents. But winning is no guarantee of staying in the nursing home. Daniel O'Connor never was able to return to the nursing home that forced him out.
A onetime first-baseman and then coach for San Francisco Bay Area minor-league baseball teams, Mr. O'Connor suffered from dementia and congestive heart failure. He had a colostomy bag, and one of his legs was amputated below the knee.
Gilroy Healthcare & Rehabilitation Center in Gilroy, Calif., sent Mr. O'Connor to the hospital in early 2006, but wouldn't take him back when doctors said he was ready to return, despite federal "bed hold" rules requiring nursing homes to give hospitalized residents first dibs on available beds.
Mr. O'Connor appealed. At a March 2006 hearing, nursing-home officials said he was argumentative, shouting and occasionally even emptying his colostomy bag on the floor in frustration. "There's probably a facility somewhere that can provide Mr. O'Connor with the treatment and the care that he needs," the nursing-home's executive director at the time told the hearing officer, according to a transcript. "It's not this one."
Hospital officials said Mr. O'Connor had arrived at the hospital with two untreated bedsores, as well as a urinary-tract infection -- conditions that "could contribute to his behavior in the facility if he was having pain," a state official testified at the hearing.
————
Begging to Return
Mr. O'Connor acknowledged being obstreperous at times, but begged to return, in part so he could attend Alcoholics Anonymous meetings in town. "I believe that there's some nurses there that can really help me out," he said.
In a ruling soon after, state hearing officer Kent Young told Gilroy Healthcare to readmit Mr. O'Connor, chastising it for ignoring federal and state bed-hold and eviction rules. State regulators fined Gilroy Healthcare $1,000, plus $50 for each day it had kept him out.
Instead of readmitting him, Gilroy Healthcare sought to overturn the decision and fines.
Dava Ashley, vice-president of California operations for Covenant Care in Aliso Viejo, Calif., which owns Gilroy Healthcare and more than 40 other nursing homes and assisted-living facilities in seven states, declined to comment on Mr. O'Connor's experience. She said company policy is to "admit patients into our facilities that we can properly take care of. We do not refuse to take them back."
Meanwhile, Mr. O'Connor remained in the hospital. His condition gradually worsened over the next 11 months. He fought off two infections and lost his other leg to amputation.
Mr. O'Connor was still in the hospital when he died in March last year. Gilroy Healthcare continues to appeal the ruling against it and can take the dispute to court if its administrative appeal fails. State officials say Gilroy Healthcare won't have to pay $14,300 in fines levied against it until all appeals are exhausted.
sidebar:
Fewer Protections With Assisted Living
In recent years, assisted-living facilities have sprung up as alternatives for those who don't quite require nursing-home care but want or need assistance with things like taking medications or bathing and dressing. Each state regulates the industry differently, so eviction policies vary. But many states simply require facilities to give four- to six-weeks' notice, with no appeal guaranteed.
In Florida, for example, the state's 2,400 assisted-living facilities must give residents 45 days' notice before evicting them, but don't need to provide a reason or appeal process, says Brian Lee, the state's long-term-care ombudsman, who pushed unsuccessfully to improve protections during the state's most recent legislative session.
"If the facility is determined to get someone out, it's generally not that hard to do it in an assisted-living facility," says Alison Hirschel, a University of Michigan Law School instructor and elder law attorney at the Michigan Poverty Law Program in Ann Arbor. "There's not much law, so they get to do what they want."
No national figures on assisted-living evictions exist, but discharge-related complaints recorded by the federal Administration on Aging more than doubled in the decade before 2006, rising 177% -- nearly twice the growth for complaints overall. Some states, including New Jersey and Washington, are pursuing assisted-living companies accused of forcing out Medicaid residents.
Some legal-aid attorneys are turning to federal fair-housing rules and the Americans with Disabilities Act to help assisted-living residents stay in their homes. They argue that those laws require all landlords, including assisted-living companies, to make reasonable accommodations for disabled residents, and prohibit them from evicting residents because their condition worsens.
"Civil rights laws apply to tenants in assisted living," says Aisha Anderson Bierma, who specializes in senior-housing issues at Legal Aid Society of Minneapolis.